Should an operation or an inpatient stay be necessary, we will carry out the registration directly from the surgery. We will inform you by telephone about your (provisional) appointment and about the necessary preliminary examinations. You will be invited to a preoperative meeting in the surgery. Here, a precise orthopedic examination and information about the planned operation, including a check of all findings, is carried out again.
Our specialists in orthopedics are affiliated doctors in the Rudolfinerhaus Hospital, in the Döbling Private Clinic, in the Hera Sanatorium and in the Evangelical Hospital. Focus: arthroscopic interventions, knee and hip endoprosthetics, foot surgery. Surgical interventions on a cash basis are primarily planned in the Hanusch Hospital or in the Ottakring Clinic (formerly Wilhelmine Hospital).
You will receive the referrals for the necessary preoperative preliminary examinations (blood draw, ECG, X-ray and surgical approval by a specialist in internal medicine) from us in the surgery.
Arthroscopic procedures
- Shoulder arthroscopy
- Knee arthroscopy
Endoprosthetics
- THA
- Knee TEP
- Shoulder TEP
Hand surgery
- Carpal tunnel syndrome
- Dupuytren’s contracture
- Flicking finger
Foot surgery
- Hallux valgus
- Toe deformities (hammer toe, claw toe)
Arthroscopic procedures
What are the benefits of an arthroscopy?
Arthroscopy is part of minimally invasive surgery that tends to cover minor injuries. Compared to the open surgical procedures, arthroscopy has the following advantages:
- Less stress on the organism
- Less pain after the procedure
- Shorter regeneration/healing times
- Faster return to everyday activities
Shoulder arthroscopy
Shoulder arthroscopy is the medical examination of the inner shoulder joint using an optical probe (arthroscope). The surgeon examines the individual structures of the shoulder joint such as muscles, ligaments and cartilage. Discomfort, pain and restricted mobility are examined. Shoulder arthroscopy is usually performed under general anesthesia, but regional anesthesia/plexus anesthesia is also possible. During the optical examination of the shoulder joint, necessary interventions can also be performed:
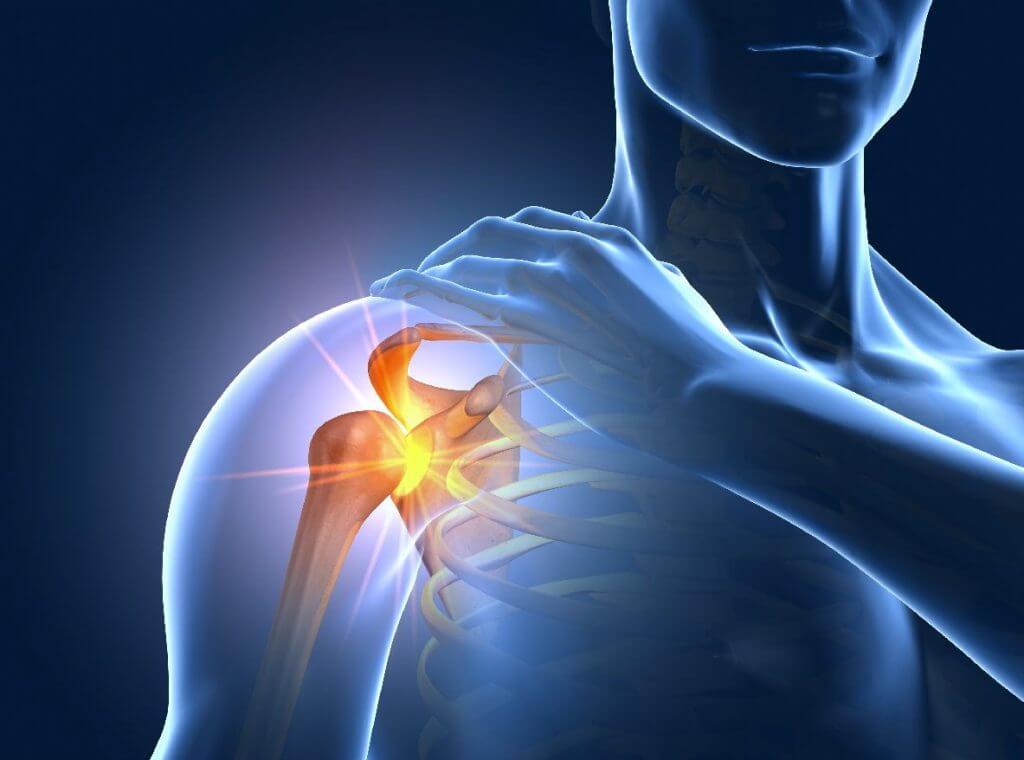
- Attachment of torn muscle tendons
- Removal of lime deposits
- Reconstruction of the shoulder muscles (so-called rotator cuff)
- Tightening of the capsule and stabilization in case of frequent shoulder dislocations
- Removal of pathologically altered parts of the joint, e.g. arthrosis
A shoulder arthroscopy can be useful for:
- Arthrosis
- Chondropathy
- Impingement syndrome
- Dislocation
Knee arthroscopy
Knee arthroscopy is a minimally invasive procedure. The operation is performed using keyhole surgery through two small skin incisions on either side of the knee. It is an operation with the smallest possible incisions. This means that the complication rate, the probability of infection and the occurrence of healing disorders after knee surgery are greatly reduced compared to so-called open surgery. The operation is performed under partial or general anesthesia. Necessary interventions can also be carried out during the optical examination of the knee joint, e.g
- Smoothing, removal or suturing of damaged parts of the meniscus
- Treatment of cartilage damage
- Treatment of cruciate ligament injuries
- Treatment of a kneecap dislocation
A knee arthroscopy can be useful for:
- Meniscus damage
- Cruciate ligament injuries
- Arthrosis in the early stages
- Cartilage damage
- Painful plica
- Free, painful joint bodies
- Problems with the kneecap (patellar luxation)
- Inflammation in the knee
Endoprosthetics
Hip TEP (total hip replacement)-artificial hip joint
Hip TEP is mostly used when the articular cartilage has worn down and arthrosis has developed. The joint head rubs in the joint socket. Osteoarthritis of the hip leads to a stiffening of the hip joint. The disease significantly affects the mobility of the patient in everyday life and the gait pattern.
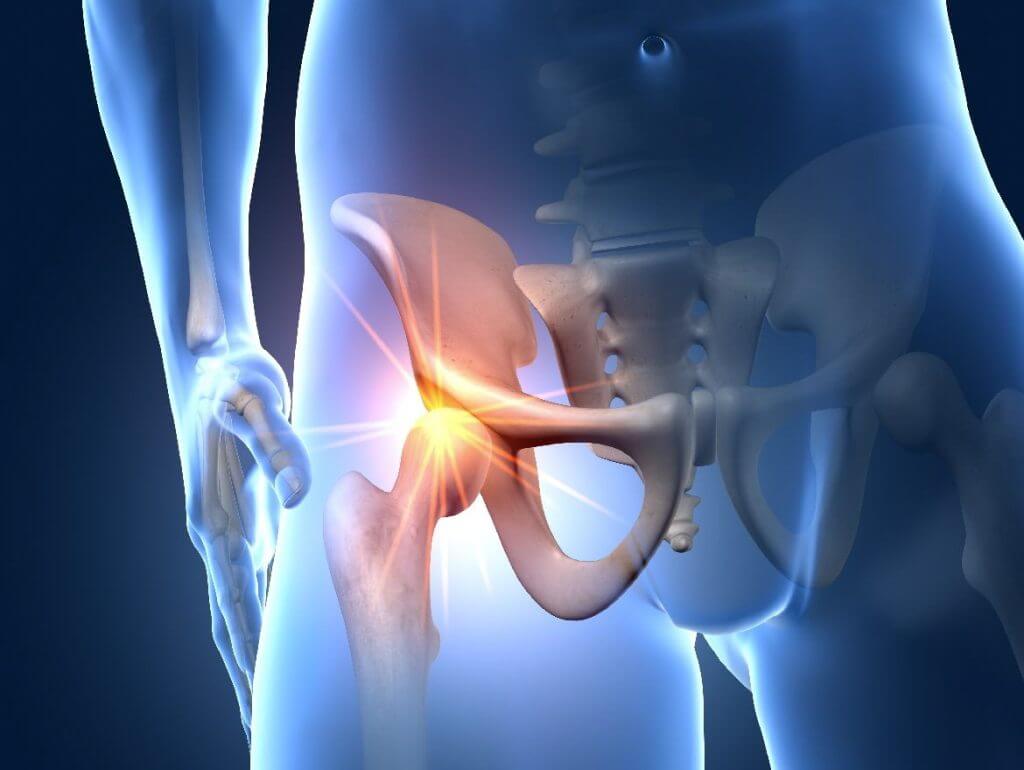
A hip prosthesis reliably restores mobility and, to a certain extent, sports ability.
Hip TEP is used for:
- Arthrosis
- Femoral neck fractures in which necrosis has developed
- Inflammatory changes in the hip joint.
- Femoral head necrosis
- Rheumatic inflammatory diseases such as arthritis
- Broken bones
Knee TEP (Total Knee Arthroplasty)-artificial knee joint
Knee TEP is mostly used when the articular cartilage has worn down and arthrosis has developed. The disease significantly affects the mobility of the patient in everyday life and the gait pattern. During the operation, the diseased part of the joint is replaced with an artificial implant.
Depending on the extent or position of the arthrosis, the entire knee joint can be replaced (knee TEP), or only the affected joint section (half slide or plain bearing prosthesis).
Knee TEP is used for:
- Arthrosis
- Cartilage damage
- Instability of the knee
- Rheumatic inflammatory diseases such as arthritis
Shoulder TEP – The artificial shoulder joint
Artificial shoulder joints have been continuously developed and successfully implanted for more than 30 years. The installation of an artificial shoulder joint has therefore become a standard procedure for the specialist. On average, around 2000 artificial shoulder joints are implanted in Austria every year, and the trend is rising.
Artificial joint replacements are only much more common in the hip and knee area, which is due to the fact that these joints have to “heave” our body weight every day and are therefore exposed to significantly higher loads.
The implantation of an artificial shoulder joint can become necessary if the wear and tear of the joint is very advanced and the patient experiences a high level of suffering despite conservative measures. Various injuries in the shoulder area such as fractures or pronounced tendon tears can also make artificial joint replacement necessary. Depending on age and indication, we have three different prosthesis models at our disposal: anatomical head replacement, anatomical replacement of the head and joint surface, and inverse shoulder prosthesis.

Which type of prosthesis is most suitable for you will be decided together with you in a precise preliminary examination. Decisive factors here include age, the severity of the arthrosis, the quality of the bone and the damage to the tendons.
All prosthesis models aim to enable the patient to regain pain-free mobility in the shoulder joint and thus improve the quality of life. A close exchange between surgeon, patient and physiotherapist is of great importance for an optimal result.
The duration of the operation is approx. 1.5 hours and can vary individually. The average postoperative hospital stay is one week. Pain therapy and passive physiotherapeutic exercise take place immediately after the procedure. The immobilisation of the arm away from the physiotherapy units is 3-6 weeks, from the 7th week free mobility is usually allowed with ongoing physiotherapy. The ability to work at a desk is possible after approx. 4-6 weeks; this time can be longer if there is heavy physical strain at work. Patients who require more intensive physiotherapeutic care also have the option of inpatient rehabilitation after the operation.
In order to achieve an ideal result, one should not wait with an artificial joint replacement until the symptoms become unbearable. Because if the arm is no longer moved for months or years due to a relieving shoulder posture, the shoulder muscles degenerate. A well-developed shoulder musculature is desirable so that the operation achieves the best possible results and the full range of motion of the shoulder prosthesis is guaranteed.
Do you have questions about conservative and surgical options in shoulder surgery? We are at your disposal and look forward to being able to help you regain freedom of movement and freedom from pain!
Hand surgery

Carpal tunnel syndrome surgery
With carpal tunnel syndrome, the median nerve (medial nerve), which runs in the wrist , is constricted. This can cause pain, tingling, numbness, and reduced mobility in the thumb, index, middle, and ring fingers. It comes among other things to nocturnal pain and weakness. The diagnosis is made based on the symptoms, nerve conduction velocity or nerve ultrasound.
During an operation under local anesthesia, the carpal ligament, which runs along the flexor side of the wrist, is severed. This relieves the median nerve. Surgery can permanently eliminate the symptoms.
Operation Dupuytren’s contracture
Dupuytren’s contracture is a benign disease of the connective tissue in the palm of the hand. An initially nodular and later cord-like thickening can lead to a permanent flexion of one or more fingers. The condition can affect any finger on either hand, most commonly the little finger and ring finger. In many cases, no cause is apparent.
If the disease has progressed so far that there are already functional limitations in the hand, surgical treatment is necessary. During an operation, the affected tissue in the hand is completely removed under local anesthesia.
Trigger finger operation
Snapping finger, or triggering finger, is a tendon-sliding disorder of the hand. This leads to narrowing of the tendon sheaths and local , nodular thickening of the affected tendon.
The sensitive flexor tendons in the hand ensure that we can bend and stretch our fingers. If the tendons thicken due to constant stress, they can no longer slide smoothly past the transverse annular ligaments. The finger snaps back into extension, which is often associated with pain. The friction causes tendonitis (tenosynovitis stenosans).
The result is that the thickened part of the tendon in the area of the annular ligament suddenly jumps past it, which causes the characteristic symptoms. The disorder usually occurs over the metatarsophalangeal joint on the inside of the hand.
In the advanced stage, it happens that the affected finger can no longer be moved independently from the bent position. During the operation under local anesthesia, the annular ligament and the pathologically altered tendon sheath are split.
Foot surgery
Foot surgery hallux valgus
We all have a hallux, it is the metatarsophalangeal joint of the big toe. Hallux valgus means that the big toe is misaligned, a deviation of the metatarsophalangeal joint of the big toe from the middle of the body. This malposition can lead to numerous complaints and is popularly known as ganglion, bunion, or frostbite. Complaints often show up as thickened and reddened skin, such as walking distances that are only short and pain-free. In the advanced stage and after conservative therapies have been exhausted, often only an operation can help.
There are many operational options. Your orthopedist will decide which one is suitable for your foot. The decision as to which operation can be carried out is made on the basis of your symptoms, after a thorough examination, an X-ray (while standing) of your foot and possibly an MRI scan.
The surgical method determines the duration and type of follow-up treatment.
Surgery hammer toe and claw toe
Claw toes and hammer toes are common toe deformities. With a hammer toe, the toe is hyperextended at the base joint and bent at the end joint, so that the toe first points up and then (like a hammer) down. Claw toes are severely overstretched in the base joint and permanently bent in the middle or end joint. The atrophied toes no longer touch the ground under load and no longer have a function when walking, balancing and compensating for uneven floors.
The surgical method is decided depending on the deformation and its extent.